Introduction
A WHO-reported hantavirus cluster aboard an Antarctic cruise ship has raised urgent questions about how a rodent-borne disease could infect eight people and lead to three deaths in one of the world’s most isolated travel settings. This article explains what is known so far about the 2026 outbreak, including where the voyage began, why transmission on a vessel poses distinct risks, and how health authorities are assessing the chance of wider spread. It also provides essential background on hantavirus, its typical sources, and the key public health issues investigators will need to resolve.
Antarctic Cruise Hantavirus Outbreak 2026: What Happened
The World Health Organization (WHO) recently issued a formal disease outbreak news report regarding a severe health event aboard a vessel navigating the Southern Ocean. During the Antarctic cruise hantavirus outbreak 2026, a total of eight passengers and crew members were confirmed infected, resulting in three fatalities. According to the WHO’s preliminary epidemiological bulletin, the cluster emerged shortly after the ship departed from a South American port, prompting an immediate medical diversion. The international health body emphasized that while the incident is tragic and requires stringent investigation, the risk of broader global dissemination remains low.
However, the confined nature of a maritime vessel presents unique epidemiological challenges that exacerbate the impact of any viral incursion. In such highly isolated maritime environments, rapid testing is crucial. Without immediate diagnostic capabilities, isolating index cases becomes exceedingly difficult, allowing pathogens to exploit the dense population dynamics and shared airflow of a modern passenger liner.
Background and definition
Hantaviruses are a family of viruses spread primarily by rodents, capable of causing severe respiratory or hemorrhagic diseases in humans. In the Americas, the pathogen typically manifests as Hantavirus Cardiopulmonary Syndrome (HCPS), an aggressive respiratory disease characterized by rapid fluid accumulation in the lungs and subsequent cardiovascular collapse. Clinical data indicates that the case fatality rate for HCPS is exceptionally high, routinely reaching 30% to 40% depending on the specific viral strain and the speed of medical intervention.
The timeline of the 2026 outbreak suggests exposure occurred either during pre-boarding activities in an endemic region or through a localized rodent infestation within the ship’s lower supply holds. Symptoms typically begin with non-specific flu-like indicators, including fever, myalgia, and fatigue, before rapidly progressing to severe shortness of breath and hypoxia within four to ten days.
Why this incident stands out
What makes this specific maritime incident historically significant is the pathogen’s suspected lineage. Health authorities have indicated that the causative agent is highly likely the Andes virus (Andes orthohantavirus). Unlike the Sin Nombre virus prevalent in North America, the Andes virus carries a unique and deeply concerning trait: it is the only known hantavirus capable of documented human-to-human transmission.
This characteristic fundamentally shifts the risk profile of the outbreak. Historically, hantavirus clusters are localized to agricultural or rural workers exposed directly to rodent habitats. An outbreak on a luxury vessel operating in sub-zero climates demonstrates how modern travel logistics can intersect with endemic zoonotic threats. The close-quarters environment of passenger decks and crew quarters provided an unprecedented vector for secondary interpersonal transmission, elevating the event from a standard localized zoonotic spillover to a complex biosecurity emergency.
Transmission, Prevention, and Onboard Response
Addressing a high-mortality viral pathogen on a moving vessel requires a multifaceted approach to both environmental control and medical triage. The Hantavirus outbreak 2026 has forced the maritime passenger industry to reevaluate baseline biosecurity protocols, particularly for vessels operating on extended itineraries far from tertiary medical facilities.
Because the incubation period for hantavirus can range anywhere from one to eight weeks, extensive contact tracing and prolonged observation are mandatory for all potentially exposed personnel. Emphasizing early diagnosis is of paramount importance; identifying the infection before severe pulmonary edema sets in is the most effective way to reduce the overall mortality rate and successfully deploy life-saving supportive care, such as extracorporeal membrane oxygenation (ECMO).
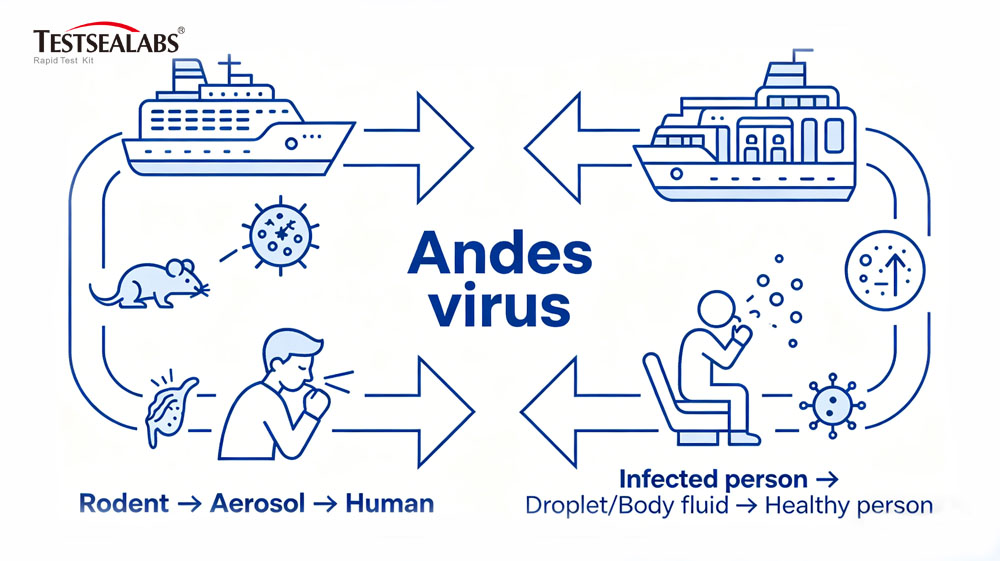
How hantavirus spreads in cruise settings
Understanding the dual pathways of transmission is essential for evaluating the rapid escalation of the cruise ship’s crisis. The primary vector involves aerosolized excreta; when fresh rodent urine, droppings, or nesting materials are disturbed, viral particles become airborne and are inhaled by human hosts. In a ship’s galley, provisioning areas, or lower storage decks, improper ventilation can inadvertently circulate these particles among the crew.
Furthermore, because this outbreak involves the Andes virus, secondary interpersonal transmission played a critical role in expanding the cluster. Close contact with infected individuals—particularly during the febrile phase—facilitates the spread through respiratory droplets or direct contact with bodily fluids, turning shared spaces into high-risk zones.
| Transmission Vector | Primary Source | Environmental Risk Factors | Estimated Incubation |
|---|---|---|---|
| Zoonotic (Rodent-borne) | Aerosolized feces, urine, saliva | Enclosed storage holds, undisturbed dust | 9 to 33 days |
| Human-to-Human | Respiratory droplets, close contact | Shared cabins, dense dining areas, medical care | 12 to 27 days |
Key prevention and containment measures
Professional containment strategies prioritize rigid environmental hygiene and rapid medical isolation. First, comprehensive integrated pest management (IPM) must be enforced, utilizing continuous trapping and structural sealing to prevent rodent ingress during port calls. Environmental decontamination requires the use of a 10% sodium hypochlorite solution or standard commercial disinfectants, as the virus is lipid-enveloped and susceptible to routine chemical breakdown. Crucially, dry sweeping or vacuuming of suspected rodent areas is strictly prohibited to prevent the aerosolization of infectious particles.
For onboard medical personnel, strict adherence to infection prevention and control (IPC) measures is non-negotiable. This includes the deployment of high-efficiency particulate air (HEPA) filters rated to capture 99.97% of airborne particles at 0.3 microns within isolation wards. Crew members handling suspected cases or cleaning potentially contaminated zones must utilize full personal protective equipment (PPE), including N95 or P100 respirators, goggles, and double gloves. Ultimately, the integration of molecular diagnostic tools into the ship’s medical bay is the definitive safeguard, ensuring that early diagnosis translates into swift isolation, targeted supportive care, and a drastically reduced case fatality rate.
Key Takeaways
- The most important conclusions and rationale for Hantavirus outbreak 2026
- Specs, compliance, and risk checks worth validating before you commit
- Practical next steps and caveats readers can apply immediately
Frequently Asked Questions
What happened in the Antarctic cruise hantavirus outbreak 2026?
WHO reported 8 confirmed infections and 3 deaths aboard an Antarctic cruise ship. The suspected virus is Andes hantavirus, which raises concern because it can spread between people.
How can hantavirus spread on a cruise ship?
Exposure may occur by inhaling aerosolized rodent urine or droppings in storage or supply areas. In this outbreak, suspected Andes virus also increased risk through close contact with infected passengers or crew.
What symptoms should exposed travelers watch for?
Watch for fever, muscle aches, fatigue, and then rapid breathing trouble or shortness of breath. Symptoms can appear 1 to 8 weeks after exposure, so monitoring should continue after disembarkation.
Why is early hantavirus testing important in outbreaks like this?
Early testing helps identify suspected cases before severe lung complications develop, supporting faster isolation, contact tracing, and supportive care. Rapid antibody screening can aid outbreak response when lab access is limited.
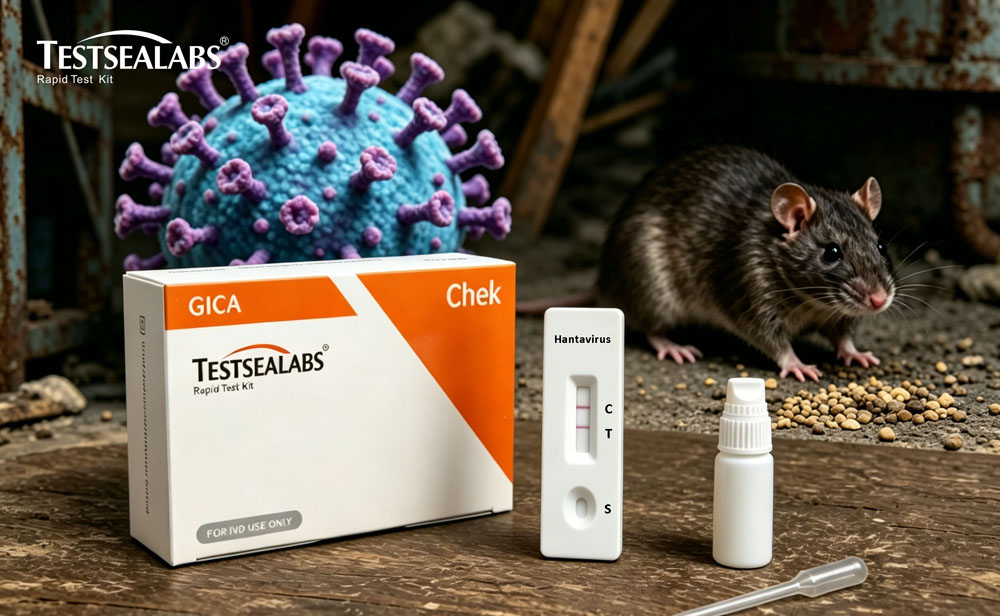
What kind of hantavirus test is relevant for emergency screening?
A hantavirus IgG/IgM rapid test kit can support quick antibody screening in clinical or outbreak settings. It should be used alongside clinical assessment and confirmatory laboratory testing, especially for high-risk exposures.
This product is intended for in vitro diagnostic use only as an initial screening tool. All positive or inconclusive results should be confirmed by a confirmatory test (e.g., RT-PCR) and clinical evaluation. The kit does not replace a medical diagnosis. Performance data are based on internal validation studies; actual results may vary. Testsea Labs recommends users follow local regulations and the manufacturer’s instructions.
Post time: May-09-2026